Cataract Surgery - How Does the Brain Process Visual Changes?
Although cataracts account for most cases of blindness worldwide, a simple surgical procedure can correct the problem and restore a patient’s vision. Cataract surgery, while fairly simple to perform, involves some cognitive adaptations that are interesting to explore.
Ocular cataracts are a common problem. In fact, research shows that more than 60% of the global population develops cataracts after the age of 75. Thus, cataracts are a significant threat as you age.
In addition, people with this eye condition suffer a progressive loss of vision that can be incapacitating.
People with cataracts have blurred vision, sensitivity to light and glare, double vision, and a whole series of visual limitations that can lead to blindness if left untreated.
What’s a cataract?
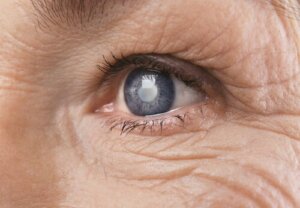
An ocular cataract is simply a clouding of the normally clear lens of your eye. The lens allows the eye to focus and is found behind the iris and the pupil.
If you have cataracts, the lens gets progressively more clouded. The clouding happens due to an accumulation of epithelial cells that change color due to different conditions.
These cells proliferate and make a physical barrier that inhibits the normal passage of light through the lens. It’s like looking through the world through a foggy windshield. Unsurprisingly, that affects normal vision.
“The only thing worse than being blind is having sight but no vision.”
-Helen Keller-
Secondary cataracts
There’s another clinical presentation of this condition, which is secondary cataracts. These are very similar to what we mentioned before. It occurs after surgery when remnants of the clouded epithelium proliferate again and cloud the lens.
The resulting symptoms are similar to the original cataract but usually less extensive. The only thing required to correct it is the elimination of this layer of tissue using a laser. It’s a quick, painless, and risk-free intervention.
About 50% of people who get cataract surgery develop secondary cataracts within a few months.
As a consequence of the formation of cataracts, the patient will experience a series of visual symptoms. The speed with which these symptoms develop depends on what kind of cataract it is. Here are some of the symptoms:
- A decrease in visual acuity.
- Sensitivity to light and glare.
- Altered chromatic perception. Colors lose intensity and blur together.
- Altered perception of the surrounding area.
In general, any change that happens as a consequence of light reflecting off of objects doesn’t properly penetrate the eye. If it does, the image is dark and distorted.
Cataracts are progressive and debilitating in nature. Especially considering that sight is possibly the most important of the six senses. Symptoms often go unnoticed at first, or patients attribute them to something else, until their vision is so affected that it’s clear that there’s an underlying problem.
A factor that can add confusion to the situation is that, while the cataract is developing, different degrees of dilation or contraction in the pupil can hide or sharpen the symptoms.
When the pupil is very dilated, much of the light that enters the eye “dodges” the cataract, and vision normalizes. If the pupil is small (in dark environments), the light hits the cataract and the patient’s vision will be very poor.
What causes cataracts?
The most widely-accepted explanation for cataracts is that it’s simply part of the body’s normal aging process. Developing cataracts is a logical consequence of reaching an advanced age. However, it’s true that only certain people actually get them.
Sometimes, the cause is genetic, in which case the condition is called congenital cataracts. Consequently, there’s a small percentage of babies who are born with this condition. It’s not usually serious, however. The surgical procedure is safe and the results tend to be quite good.
Aside from the above and idiopathic cataracts (that have an unknown origin), there are three other possible causes of cataracts:
- A high degree of myopia (nearsightedness) that has an influence on the ocular morphology.
- Eye injuries.
- Long-term use of steroid-based medications, especially corticoids. The chronic use of cortisone in patients with rheumatism or allergy medications in patients with allergies are two examples.
Whatever the cause, cataracts affect an individual’s daily life to such a degree that they can cause anxiety and depression.
“Vision is the art of seeing what is invisible to others.”
-Jonathan Swift-
What happens during cataract surgery?
It’s considered a simple, safe, and outpatient surgical intervention. As a result, there’s no need to be afraid. Doctors around the world do these procedures hundreds of times a day, and the success rate is extremely high.
In a nutshell, the surgery involves the physical extraction of the cataract using an instrument that the doctor inserts into the front of the eyeball.
Because the tissue that the doctor removes is next to the healthy tissue that makes up the lens, they have to remove the lens completely or partially. As a result, the eye is left unable to focus on its own. After all, it’s the lens that allows you to focus on things and adjust your sight.
To make up for that structural and functional deficiency, the doctor implants an intraocular lens in the space that was previously occupied. This tiny lens allows the eye to focus and has characteristics that complement the lens in the other eye.
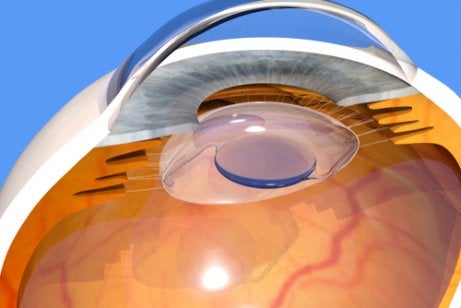
This is true because cataracts are almost always bilateral. In other words, they happen in both eyes at the same time. Together, they form light projections focused on the retina level that’ll then give way to the visual representation in the brain.
Performance of intraocular lenses
As you can imagine, artificial intraocular lenses don’t perform as well as your natural lenses. Intraocular lenses are fixed and they don’t have the ability to change their shape to focus and unfocus. That deeply alters the way a person sees on many different levels.
The brain, which is responsible for producing a final perceptive image, has to adapt to this new way of taking in light and transforming images. That’s why it takes some cataract surgery patients up to a month to readjust. While the process is taking place, their vision is just as inaccurate and uncomfortable as it was before.
Thanks to brain plasticity and the ability of your neural systems to reorganize, adapt, and recover lost functionality, when the adjustment period is over, the patient’s vision will be fairly normal.
Next, we’ll talk about a series of components of the visual process that are affected by cataract surgery. These are changes that the brain learns to correct in order to have the most effective visual system possible.
Changes that the brain has to learn to process
Permanent focus and elimination of focus time
The intraocular lens focuses but can’t change the degree of that focus. Consequently, from the moment you open your eyes, you can see in a focused way at any distance, near or far. There’s no need to squint your eyes or let milliseconds pass while your gaze switches focus from one thing to the next.
This feels very strange at first, but over time your brain adapts to the distortion.
The need for more light to be able to see properly
If you have cataracts, you probably avoid brightly-lit spaces. That’s because they dilate the pupil and cause visual disturbances. After cataract surgery (implantation of the intraocular lens), however, the better the light, the better you’ll be able to see.
This occurs because the artificial lens doesn’t cover the entire diameter of the pupil when it’s fully dilated (which happens in dark places). When the pupil fully dilates, some of the light enters the eye outside the intraocular lens which causes blurriness or double vision.
The need for physical orientation
Given that intraocular lenses can’t adjust their focus if you want your vision to adjust to objects at different distances you have to actually move your body. You can move forward or back and move your head around at different angles to find the spot that allows you to see the object most clearly.
Residual farsightedness
In general, intraocular lenses are better at focusing on middle and long distances and less efficient at short distances. As a result, after cataract surgery, patients often need glasses to see things that are close.

Visual changes during physical exertion
Intraocular lenses aren’t quite as stable in the eye as your natural lens. Consequently, variations in intraocular tension, the pressure of the fluid inside your eye, caused by physical exertion can cause the lens to shift very slightly. Those small movements distort your vision.
Eye irritation
Because the ocular lens (or conjunctival) epithelium is perforated during surgery, it develops microscopic scarring that increases sensitivity to irritants such as smoke or dust, etc.
Different visual convergence
The image that your brain processes is captured thanks to the fusion of two images of the same object, one from each eye.
Because intraocular lenses are in a different position than the original lens, the exact point in the retina where the light is projected is also different.
In that sense, the two images that fuse to form the final image come from two different places. The brain has to re-learn to fuse them together in an effective way.
Distortion of the visual plane and object size
Implanted intraocular lenses usually cause a flatter visual field. The objects in your field of vision tend to appear less rounded.
They also tend to slightly shrink the image that you focus on, which means that everything looks a little bit smaller than before. The brain has to adjust to this change as well to avoid triggering visual discomfort.
The presence of visual artifacts
In medicine, an artifact is the presence of an element that doesn’t occur naturally in that particular place. In ophthalmology, a visual artifact is an element that shows up in the workings of the visual system that shouldn’t be there.
People with intraocular lenses sometimes perceive components or movement of the lens itself.
This can be uncomfortable and disconcerting. It also requires a certain amount of energy as your brain tries to deal with the incongruence. The good news is that cerebral plasticity once again saves the day, and, after a time, these problems will resolve themselves.
If you’ve had cataracts before or you think you might have them in the future, this is important (and interesting) information that’ll help you be a more informed and prepared patient.
Although cataracts account for most cases of blindness worldwide, a simple surgical procedure can correct the problem and restore a patient’s vision. Cataract surgery, while fairly simple to perform, involves some cognitive adaptations that are interesting to explore.
Ocular cataracts are a common problem. In fact, research shows that more than 60% of the global population develops cataracts after the age of 75. Thus, cataracts are a significant threat as you age.
In addition, people with this eye condition suffer a progressive loss of vision that can be incapacitating.
People with cataracts have blurred vision, sensitivity to light and glare, double vision, and a whole series of visual limitations that can lead to blindness if left untreated.
What’s a cataract?
An ocular cataract is simply a clouding of the normally clear lens of your eye. The lens allows the eye to focus and is found behind the iris and the pupil.
If you have cataracts, the lens gets progressively more clouded. The clouding happens due to an accumulation of epithelial cells that change color due to different conditions.
These cells proliferate and make a physical barrier that inhibits the normal passage of light through the lens. It’s like looking through the world through a foggy windshield. Unsurprisingly, that affects normal vision.
“The only thing worse than being blind is having sight but no vision.”
-Helen Keller-

Secondary cataracts
There’s another clinical presentation of this condition, which is secondary cataracts. These are very similar to what we mentioned before. It occurs after surgery when remnants of the clouded epithelium proliferate again and cloud the lens.
The resulting symptoms are similar to the original cataract but usually less extensive. The only thing required to correct it is the elimination of this layer of tissue using a laser. It’s a quick, painless, and risk-free intervention.
About 50% of people who get cataract surgery develop secondary cataracts within a few months.
As a consequence of the formation of cataracts, the patient will experience a series of visual symptoms. The speed with which these symptoms develop depends on what kind of cataract it is. Here are some of the symptoms:
- A decrease in visual acuity.
- Sensitivity to light and glare.
- Altered chromatic perception. Colors lose intensity and blur together.
- Altered perception of the surrounding area.
In general, any change that happens as a consequence of light reflecting off of objects doesn’t properly penetrate the eye. If it does, the image is dark and distorted.
Cataracts are progressive and debilitating in nature. Especially considering that sight is possibly the most important of the six senses. Symptoms often go unnoticed at first, or patients attribute them to something else, until their vision is so affected that it’s clear that there’s an underlying problem.
A factor that can add confusion to the situation is that, while the cataract is developing, different degrees of dilation or contraction in the pupil can hide or sharpen the symptoms.
When the pupil is very dilated, much of the light that enters the eye “dodges” the cataract, and vision normalizes. If the pupil is small (in dark environments), the light hits the cataract and the patient’s vision will be very poor.
What causes cataracts?
The most widely-accepted explanation for cataracts is that it’s simply part of the body’s normal aging process. Developing cataracts is a logical consequence of reaching an advanced age. However, it’s true that only certain people actually get them.
Sometimes, the cause is genetic, in which case the condition is called congenital cataracts. Consequently, there’s a small percentage of babies who are born with this condition. It’s not usually serious, however. The surgical procedure is safe and the results tend to be quite good.
Aside from the above and idiopathic cataracts (that have an unknown origin), there are three other possible causes of cataracts:
- A high degree of myopia (nearsightedness) that has an influence on the ocular morphology.
- Eye injuries.
- Long-term use of steroid-based medications, especially corticoids. The chronic use of cortisone in patients with rheumatism or allergy medications in patients with allergies are two examples.
Whatever the cause, cataracts affect an individual’s daily life to such a degree that they can cause anxiety and depression.
“Vision is the art of seeing what is invisible to others.”
-Jonathan Swift-
What happens during cataract surgery?
It’s considered a simple, safe, and outpatient surgical intervention. As a result, there’s no need to be afraid. Doctors around the world do these procedures hundreds of times a day, and the success rate is extremely high.
In a nutshell, the surgery involves the physical extraction of the cataract using an instrument that the doctor inserts into the front of the eyeball.
Because the tissue that the doctor removes is next to the healthy tissue that makes up the lens, they have to remove the lens completely or partially. As a result, the eye is left unable to focus on its own. After all, it’s the lens that allows you to focus on things and adjust your sight.
To make up for that structural and functional deficiency, the doctor implants an intraocular lens in the space that was previously occupied. This tiny lens allows the eye to focus and has characteristics that complement the lens in the other eye.

This is true because cataracts are almost always bilateral. In other words, they happen in both eyes at the same time. Together, they form light projections focused on the retina level that’ll then give way to the visual representation in the brain.
Performance of intraocular lenses
As you can imagine, artificial intraocular lenses don’t perform as well as your natural lenses. Intraocular lenses are fixed and they don’t have the ability to change their shape to focus and unfocus. That deeply alters the way a person sees on many different levels.
The brain, which is responsible for producing a final perceptive image, has to adapt to this new way of taking in light and transforming images. That’s why it takes some cataract surgery patients up to a month to readjust. While the process is taking place, their vision is just as inaccurate and uncomfortable as it was before.
Thanks to brain plasticity and the ability of your neural systems to reorganize, adapt, and recover lost functionality, when the adjustment period is over, the patient’s vision will be fairly normal.
Next, we’ll talk about a series of components of the visual process that are affected by cataract surgery. These are changes that the brain learns to correct in order to have the most effective visual system possible.
Changes that the brain has to learn to process
Permanent focus and elimination of focus time
The intraocular lens focuses but can’t change the degree of that focus. Consequently, from the moment you open your eyes, you can see in a focused way at any distance, near or far. There’s no need to squint your eyes or let milliseconds pass while your gaze switches focus from one thing to the next.
This feels very strange at first, but over time your brain adapts to the distortion.
The need for more light to be able to see properly
If you have cataracts, you probably avoid brightly-lit spaces. That’s because they dilate the pupil and cause visual disturbances. After cataract surgery (implantation of the intraocular lens), however, the better the light, the better you’ll be able to see.
This occurs because the artificial lens doesn’t cover the entire diameter of the pupil when it’s fully dilated (which happens in dark places). When the pupil fully dilates, some of the light enters the eye outside the intraocular lens which causes blurriness or double vision.
The need for physical orientation
Given that intraocular lenses can’t adjust their focus if you want your vision to adjust to objects at different distances you have to actually move your body. You can move forward or back and move your head around at different angles to find the spot that allows you to see the object most clearly.
Residual farsightedness
In general, intraocular lenses are better at focusing on middle and long distances and less efficient at short distances. As a result, after cataract surgery, patients often need glasses to see things that are close.

Visual changes during physical exertion
Intraocular lenses aren’t quite as stable in the eye as your natural lens. Consequently, variations in intraocular tension, the pressure of the fluid inside your eye, caused by physical exertion can cause the lens to shift very slightly. Those small movements distort your vision.
Eye irritation
Because the ocular lens (or conjunctival) epithelium is perforated during surgery, it develops microscopic scarring that increases sensitivity to irritants such as smoke or dust, etc.
Different visual convergence
The image that your brain processes is captured thanks to the fusion of two images of the same object, one from each eye.
Because intraocular lenses are in a different position than the original lens, the exact point in the retina where the light is projected is also different.
In that sense, the two images that fuse to form the final image come from two different places. The brain has to re-learn to fuse them together in an effective way.
Distortion of the visual plane and object size
Implanted intraocular lenses usually cause a flatter visual field. The objects in your field of vision tend to appear less rounded.
They also tend to slightly shrink the image that you focus on, which means that everything looks a little bit smaller than before. The brain has to adjust to this change as well to avoid triggering visual discomfort.
The presence of visual artifacts
In medicine, an artifact is the presence of an element that doesn’t occur naturally in that particular place. In ophthalmology, a visual artifact is an element that shows up in the workings of the visual system that shouldn’t be there.
People with intraocular lenses sometimes perceive components or movement of the lens itself.
This can be uncomfortable and disconcerting. It also requires a certain amount of energy as your brain tries to deal with the incongruence. The good news is that cerebral plasticity once again saves the day, and, after a time, these problems will resolve themselves.
If you’ve had cataracts before or you think you might have them in the future, this is important (and interesting) information that’ll help you be a more informed and prepared patient.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Taylor HR. Cataract: how much surgery do we have to do? Br J Ophthalmol 2000; 84: 1-2.
- McCarty CA, Keeffe JE, Taylor HR. The need for cataract surgery: projections based on lens opacity, visual acuity, and personal concern. Br J Ophthalmol 1999; 83: 62 – 65.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.







