What Are Benzodiazepines? Uses and Consequences


Written and verified by the psychologist Valeria Sabater
In the great movie, “August: Osage County,” they said that women generally dissolve their problems with pills, while men do it with alcohol. In the movie we see Meryl Streep powerfully showing us what consistent, uncontrolled consumption of benzodiazepines can look like.
Sleeping pills pushed by doctors as an easy, quick, and cheap way to alleviate the existential suffering of their patients.
The movie paints a very grim, but truthful, picture. An all-too-common one: people addicted to a legal drug prescribed by their doctors. Patients who need higher doses every day in order to feel good. Or even old women who’ve taken their “little” sleeping pill for decades and now suffer through a lower quality of life than they deserve.
There’s a lot of darkness surrounding hypnosedatives and their supposed purpose of making our lives more manageable when things are hard. Whether they’re real or imaginary.
No one doubts their effectiveness in the short term, because they do work. But as we already know, anxiety and depression can last an extremely long time. That’s where the risk lies. That’s where we get the dependence and side effects that we really can’t ignore any longer.
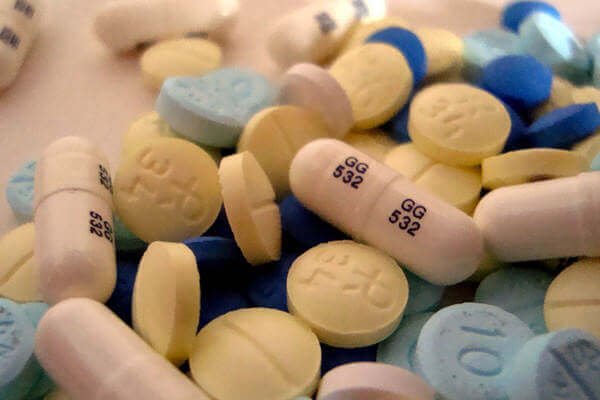
What are benzodiazepines?
A lot of people won’t recognize the word “benzodiazepines” at all. But if we say Orfidal, Tranxilium, Lorazepam, Lexatin, Valium, or Trankimazin, things change. Because a large part of the population has taken them for some reason or another or at least has a family member, friend, or coworker who needs them every day.
Okay then, but…what really are benzodiazepines?
- Benzodiazepines act like sedatives (they slow down bodily functions).
- Also, they’re psychotropic medicines that have an effect on the central nervous system. That is, their effects aren’t just limited to relaxing or sedating us. They’re anticonvulsants, amnesiants, and myorelaxants.
- They work by increasing the effect of a brain chemical called GABA (gamma-aminobutyric-acid).
- GABA is a brain inhibitor that’s made in the cerebellum, the basal ganglia, and a lot of parts of the spinal cord. Its function is to relax and reduce the activity of our neurons.
As a side note, it’s worth adding that benzodiazepines entered the pharmaceutical market in the 60’s as a replacement for barbiturates. Since then, and with the launch of the pharmaceutical company, ROCHE, in 1963, maker of the well-known drug Valium (diazepam), benzodiazepines have become the most consumed prescription “drug” of all time.
The consumption of minor mood-altering drugs, such as tranquilizers, has gone up 20% worldwide this year.
Uses and types of benzodiazepines
We use benzodiazepines to treat panic or generalized anxiety disorders. We use them for insomnia, alcohol withdrawal, epilepsy, affective disorders, after surgery, and even to alleviate withdrawal symptoms from other drugs.
Also, as shown by various studies, like the one done at the Department of Health Sciences at the University of San Jorge, Zaragoza (Spain), benzodiazepines are being prescribed more and more in retirement communities.
It’s an important fact that makes specialists ask themselves if the clinical benefits of these drugs make up for their negative side effects.
On the other hand, it’s worth repeating once again that it’s medication that you can only take with doctor’s prescription. And whether they can be taken alongside antidepressants or anti-psychotics, it will always be a specialist who prescribes them and controls the dose.

Types of benzodiazepines
Benzodiazepines are classified based on their half-life in our bodies. Now let’s look at them in more detail.
Prolonged duration, between 40 and 200 hours.
- Clobazam.
- Clorazepate.
- Chlordiazepoxide.
- Diazepam.
- Flurazepam.
- Medazepam.
- Phenazepam.
- Clotiazepam.
- Prazepam.
Medium duration, between 20 and 40 hours.
- Clonazepam
- Bromazepam.
- Flunitrazepam.
- Nitrazepam.
Short duration, between 5 and 20 hours.
- Alprazolam.
- Lormetazepam.
- Lorazepam.
- Oxazepam.
Reduced duration, between 1 and 5 hours.
- Brotizolam.
- Midazolam
Effects associated with benzodiazepines
Benzodiazepines are effective. They never fail, they give us uninterrupted rest, alleviate that desperate suffering after a breakup, and even help us make our workdays more manageable.
But everything in life has a price, and with this drug, sometimes it’s like making a pact with the devil. We shouldn’t use them for more than 4 or 6 weeks. Otherwise, there’s a good chance we will start to form a dependence.
However, life keeps on hurting, problems keep weighing us down, insomnia keeps visiting us, and anxiety keeps on devouring us. We ask our doctor for help and since he doesn’t have anything else to offer, he gives in. Then the slow and devastating addiction begins.

Common physical side effects of benzodiazepine addiction
- Drowsiness.
- Dizziness.
- Confusion.
- Loss of balance (especially in the elderly.
- Trouble speaking.
- Muscular weakness.
- Constipation
- Nausea.
- Dry mouth.
- Blurry vision.
Progressive effects on memory associated with benzodiazepine consumption
Benzodiazepines have a notably reduce our ability to take in new information. And also, prolonged use leads to evident difficulty in cognitive processes. It’s hard for us to concentrate, solve problems, deduce information, put ideas together…
Paradoxical effects
A “paradoxical reaction to a medication” is the appearance of an outcome that’s the opposite of what’s intended. There are a lot of patients who, after spending months or even years taking some kind of benzodiazepine, start to feel some or many of these symptoms:
- Increase in anxiety.
- Feelings of anger or rage.
- Agitation.
- Melancholy.
- Depersonalization (feeling of indifference towards their surroundings).
- Depression.
- Derealization (feeling that their surroundings aren’t real).
- Hallucinations.
- Nightmares.
- Changes in personality.
- Psychosis.
- Restlessness.
- Suicidal behavior or thoughts.
Benzodiazepines in people over 60
Primary care doctors tend to prescribe short-duration benzodiazepines for treating insomnia in people over 60. It’s a common practice, and has the goal of improving their quality of sleep, with the end goal of better quality of life. But, there are a lot of studies that warn of the different risks associated with prolonged consumption of these medications in elderly patients:
- Alterations in cognition and memory.
- Increase in risk of falling and its consequences (like hip fractures).
- Greater likelihood of car accidents.
- The use of benzodiazepines can also be an early indicator when it comes to developing dementia.
All this brings us to a very clear conclusion to reflect on. The unjustified, long-term use of these medications should be seen as a public health issue.
Laura and the story of doctor-prescribed addiction
Laura is 39 years old, has a 3-year-old and an 8-year-old, and works for a public relations firm. It’s a good job, with a lot of pressure, goals to accomplish, and a business to get on the market. There are days when it’s really hard to do it all: to be a mother, a successful creative person, all while managing anxiety.
“Regular consumption of benzodiazepines creates long-term addiction, instead of treating the problem or the illness.”

A few weeks ago she had to check into a hospital because of intense withdrawal symptoms. It all started with some buzzing in her ears. She couldn’t focus on anything else, just that persistent tinnitus. Next came the tingling in her arms and feet, feeling like her mouth was burning, and that awful sensitivity to light.
It changed her mood, just like that. That was when her children started to be afraid of her. That was when the world started to go off kilter and life got out of sync. Nothing fit in her mind and all she felt was the desire to hide somewhere she could disappear, fade away, and dissolve into nothing.
When she realized she was addicted to the benzodiazepines, she couldn’t believe it. It’s extremely hard to come to terms with the fact that it’s possible to develop an addiction to a medication our doctors prescribed. But, the processes of anxiety and depression are long and our time in the doctor’s office is short. Under these circumstances, at times, it can be complicated to properly manage the drugs.
Laura and her attempt to stop taking benzodiazepines
Laura tried to get off them. However, soon she found that was impossible, because the effects are devastating. Life isn’t a straight path, but actually a long, zig-zagging uphill battle. So, sometimes we need help from those little pills. The little pills that take away our pain and put us to sleep.
But, benzodiazepine addiction is similar to heroin, and sometimes there’s no choice but to go to a treatment center for advanced stages of addiction.
Easy but dangerous, cheap but so costly
We can’t put all the responsibility on our doctors. Because the organization, the system, and the politics that shape our environments don’t encourage that personalized attention that proper diagnosis and treatment require.
Also, other factors like unemployment, bad jobs, the recession, poverty, feelings of loneliness, and poor emotional management can make things worse and push us towards medication.
To conclude, we want to remind people that benzodiazepines are effective in the short-term. Beyond that, we need other strategies, other approaches to untie the knot of our lives: psychotherapy, personal willpower, and authentic, sensible, and empathetic support from people around us. We can do it.
Bibliographic references
-Andrés-Trelles, F. (1993) Fármacos utilizados en la ansiedad: benzodiacepinas y otros ansiolíticos. Madrid: MacGraw Hill Interamericana.
-Hardman J. G., Goodman L. S., Gilman A. (1995) The Pharmacological Basis of Therapeutics. Pages. 385-398. New York, MacGraw-Hill.
-Robert Whitaker, (2010) Anatomy of an Epidemic. Crown Publishing Group.
-Sophie Billioti, Yola Moride , Thierry Ducruet (9-09-2014) Benzodiazepine use and risk of Alzheimer’s disease: case-control study. British Medical Journal, 349, págs 205-206
Eugene Rubin, Charles Zorumski, (2015) How Many People Take Benzodiazepines? Psychology Today https://www.psychologytoday.com/blog/demystifying-psychiatry/201505/how-many-people-take-benzodiazepines
In the great movie, “August: Osage County,” they said that women generally dissolve their problems with pills, while men do it with alcohol. In the movie we see Meryl Streep powerfully showing us what consistent, uncontrolled consumption of benzodiazepines can look like.
Sleeping pills pushed by doctors as an easy, quick, and cheap way to alleviate the existential suffering of their patients.
The movie paints a very grim, but truthful, picture. An all-too-common one: people addicted to a legal drug prescribed by their doctors. Patients who need higher doses every day in order to feel good. Or even old women who’ve taken their “little” sleeping pill for decades and now suffer through a lower quality of life than they deserve.
There’s a lot of darkness surrounding hypnosedatives and their supposed purpose of making our lives more manageable when things are hard. Whether they’re real or imaginary.
No one doubts their effectiveness in the short term, because they do work. But as we already know, anxiety and depression can last an extremely long time. That’s where the risk lies. That’s where we get the dependence and side effects that we really can’t ignore any longer.

What are benzodiazepines?
A lot of people won’t recognize the word “benzodiazepines” at all. But if we say Orfidal, Tranxilium, Lorazepam, Lexatin, Valium, or Trankimazin, things change. Because a large part of the population has taken them for some reason or another or at least has a family member, friend, or coworker who needs them every day.
Okay then, but…what really are benzodiazepines?
- Benzodiazepines act like sedatives (they slow down bodily functions).
- Also, they’re psychotropic medicines that have an effect on the central nervous system. That is, their effects aren’t just limited to relaxing or sedating us. They’re anticonvulsants, amnesiants, and myorelaxants.
- They work by increasing the effect of a brain chemical called GABA (gamma-aminobutyric-acid).
- GABA is a brain inhibitor that’s made in the cerebellum, the basal ganglia, and a lot of parts of the spinal cord. Its function is to relax and reduce the activity of our neurons.
As a side note, it’s worth adding that benzodiazepines entered the pharmaceutical market in the 60’s as a replacement for barbiturates. Since then, and with the launch of the pharmaceutical company, ROCHE, in 1963, maker of the well-known drug Valium (diazepam), benzodiazepines have become the most consumed prescription “drug” of all time.
The consumption of minor mood-altering drugs, such as tranquilizers, has gone up 20% worldwide this year.
Uses and types of benzodiazepines
We use benzodiazepines to treat panic or generalized anxiety disorders. We use them for insomnia, alcohol withdrawal, epilepsy, affective disorders, after surgery, and even to alleviate withdrawal symptoms from other drugs.
Also, as shown by various studies, like the one done at the Department of Health Sciences at the University of San Jorge, Zaragoza (Spain), benzodiazepines are being prescribed more and more in retirement communities.
It’s an important fact that makes specialists ask themselves if the clinical benefits of these drugs make up for their negative side effects.
On the other hand, it’s worth repeating once again that it’s medication that you can only take with doctor’s prescription. And whether they can be taken alongside antidepressants or anti-psychotics, it will always be a specialist who prescribes them and controls the dose.

Types of benzodiazepines
Benzodiazepines are classified based on their half-life in our bodies. Now let’s look at them in more detail.
Prolonged duration, between 40 and 200 hours.
- Clobazam.
- Clorazepate.
- Chlordiazepoxide.
- Diazepam.
- Flurazepam.
- Medazepam.
- Phenazepam.
- Clotiazepam.
- Prazepam.
Medium duration, between 20 and 40 hours.
- Clonazepam
- Bromazepam.
- Flunitrazepam.
- Nitrazepam.
Short duration, between 5 and 20 hours.
- Alprazolam.
- Lormetazepam.
- Lorazepam.
- Oxazepam.
Reduced duration, between 1 and 5 hours.
- Brotizolam.
- Midazolam
Effects associated with benzodiazepines
Benzodiazepines are effective. They never fail, they give us uninterrupted rest, alleviate that desperate suffering after a breakup, and even help us make our workdays more manageable.
But everything in life has a price, and with this drug, sometimes it’s like making a pact with the devil. We shouldn’t use them for more than 4 or 6 weeks. Otherwise, there’s a good chance we will start to form a dependence.
However, life keeps on hurting, problems keep weighing us down, insomnia keeps visiting us, and anxiety keeps on devouring us. We ask our doctor for help and since he doesn’t have anything else to offer, he gives in. Then the slow and devastating addiction begins.

Common physical side effects of benzodiazepine addiction
- Drowsiness.
- Dizziness.
- Confusion.
- Loss of balance (especially in the elderly.
- Trouble speaking.
- Muscular weakness.
- Constipation
- Nausea.
- Dry mouth.
- Blurry vision.
Progressive effects on memory associated with benzodiazepine consumption
Benzodiazepines have a notably reduce our ability to take in new information. And also, prolonged use leads to evident difficulty in cognitive processes. It’s hard for us to concentrate, solve problems, deduce information, put ideas together…
Paradoxical effects
A “paradoxical reaction to a medication” is the appearance of an outcome that’s the opposite of what’s intended. There are a lot of patients who, after spending months or even years taking some kind of benzodiazepine, start to feel some or many of these symptoms:
- Increase in anxiety.
- Feelings of anger or rage.
- Agitation.
- Melancholy.
- Depersonalization (feeling of indifference towards their surroundings).
- Depression.
- Derealization (feeling that their surroundings aren’t real).
- Hallucinations.
- Nightmares.
- Changes in personality.
- Psychosis.
- Restlessness.
- Suicidal behavior or thoughts.
Benzodiazepines in people over 60
Primary care doctors tend to prescribe short-duration benzodiazepines for treating insomnia in people over 60. It’s a common practice, and has the goal of improving their quality of sleep, with the end goal of better quality of life. But, there are a lot of studies that warn of the different risks associated with prolonged consumption of these medications in elderly patients:
- Alterations in cognition and memory.
- Increase in risk of falling and its consequences (like hip fractures).
- Greater likelihood of car accidents.
- The use of benzodiazepines can also be an early indicator when it comes to developing dementia.
All this brings us to a very clear conclusion to reflect on. The unjustified, long-term use of these medications should be seen as a public health issue.
Laura and the story of doctor-prescribed addiction
Laura is 39 years old, has a 3-year-old and an 8-year-old, and works for a public relations firm. It’s a good job, with a lot of pressure, goals to accomplish, and a business to get on the market. There are days when it’s really hard to do it all: to be a mother, a successful creative person, all while managing anxiety.
“Regular consumption of benzodiazepines creates long-term addiction, instead of treating the problem or the illness.”

A few weeks ago she had to check into a hospital because of intense withdrawal symptoms. It all started with some buzzing in her ears. She couldn’t focus on anything else, just that persistent tinnitus. Next came the tingling in her arms and feet, feeling like her mouth was burning, and that awful sensitivity to light.
It changed her mood, just like that. That was when her children started to be afraid of her. That was when the world started to go off kilter and life got out of sync. Nothing fit in her mind and all she felt was the desire to hide somewhere she could disappear, fade away, and dissolve into nothing.
When she realized she was addicted to the benzodiazepines, she couldn’t believe it. It’s extremely hard to come to terms with the fact that it’s possible to develop an addiction to a medication our doctors prescribed. But, the processes of anxiety and depression are long and our time in the doctor’s office is short. Under these circumstances, at times, it can be complicated to properly manage the drugs.
Laura and her attempt to stop taking benzodiazepines
Laura tried to get off them. However, soon she found that was impossible, because the effects are devastating. Life isn’t a straight path, but actually a long, zig-zagging uphill battle. So, sometimes we need help from those little pills. The little pills that take away our pain and put us to sleep.
But, benzodiazepine addiction is similar to heroin, and sometimes there’s no choice but to go to a treatment center for advanced stages of addiction.

Easy but dangerous, cheap but so costly
We can’t put all the responsibility on our doctors. Because the organization, the system, and the politics that shape our environments don’t encourage that personalized attention that proper diagnosis and treatment require.
Also, other factors like unemployment, bad jobs, the recession, poverty, feelings of loneliness, and poor emotional management can make things worse and push us towards medication.
To conclude, we want to remind people that benzodiazepines are effective in the short-term. Beyond that, we need other strategies, other approaches to untie the knot of our lives: psychotherapy, personal willpower, and authentic, sensible, and empathetic support from people around us. We can do it.
Bibliographic references
-Andrés-Trelles, F. (1993) Fármacos utilizados en la ansiedad: benzodiacepinas y otros ansiolíticos. Madrid: MacGraw Hill Interamericana.
-Hardman J. G., Goodman L. S., Gilman A. (1995) The Pharmacological Basis of Therapeutics. Pages. 385-398. New York, MacGraw-Hill.
-Robert Whitaker, (2010) Anatomy of an Epidemic. Crown Publishing Group.
-Sophie Billioti, Yola Moride , Thierry Ducruet (9-09-2014) Benzodiazepine use and risk of Alzheimer’s disease: case-control study. British Medical Journal, 349, págs 205-206
Eugene Rubin, Charles Zorumski, (2015) How Many People Take Benzodiazepines? Psychology Today https://www.psychologytoday.com/blog/demystifying-psychiatry/201505/how-many-people-take-benzodiazepines
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- -Andrés-Trelles, F. (1993) Fármacos utilizados en la ansiedad: benzodiacepinas y otros ansiolíticos. Madrid: MacGraw Hill Interamericana.
- -Hardman J. G., Goodman L. S., Gilman A. (1996) Las bases farmacológicas de la terapéutica. Vol. I. Págs. 385-398. Madrid: MacGraw-Hill Interamericana.
- -Robert Whitaker, (2015) Anatomía de una epidemia, Madrid: Capitán Swing
- -Sophie Billioti, Yola Moride , Thierry Ducruet (9-09-2014) Benzodiazepine use and risk of Alzheimer’s disease: case-control study. British Medical Journal, 349, págs 205-206
- Eugene Rubin, Charles Zorumski, (2015) How Many People Take Benzodiazepines? Psichology Today https://www.psychologytoday.com/blog/demystifying-psychiatry/201505/how-many-people-take-benzodiazepines
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.







