Vascular Dementia: Characteristics and Treatment


Written and verified by the psychologist Valeria Sabater
Vascular dementia is, after Alzheimer’s, the most common neurodegenerative condition after the age of 70. The origin of this condition lies in blood flow problems, which make it difficult for blood to reach the brain. It’s somewhat slow and progressive but is something that greatly impacts a person’s quality of life, affecting their memory, movements, and communication.
We should note that, sadly, vascular dementia isn’t a reversible condition. Unfortunately, there’s no treatment to stop or effectively treat this harsh reality that hundreds of people and their families live. However, we can slow down its effects.
We should highlight one aspect at this point. Unlike Alzheimer’s, this type of dementia does have certain protective or precipitating factors, depending on the context, which we can all, to some extent, control.
This doesn’t mean that we can avoid it 100 percent, but it does mean that we can reduce its probability or delay its onset. We can relate vascular dementia to such well-known underlying factors as high blood pressure, cholesterol and triglycerides, diabetes, excess weight, an unhealthy lifestyle, etc.
Therefore, improving your vascular health is within your reach. We’re now going to have a look at the characteristics that define this disease, which accounts for about 20 percent of all dementia diagnoses.
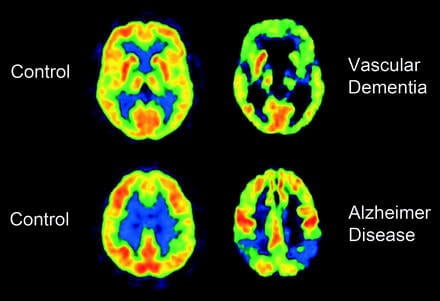
Vascular dementia is the result of a repeated series of small strokes over time, which eventually lead to cognitive, mobility, and communication problems.
What’s vascular dementia?
Vascular dementia is a neurodegenerative disease that causes cognitive impairment. The origin lies in various vascular lesions and alterations, the most common being the following:
- A narrowing of the blood vessels in the brain, as a result of arteriosclerosis.
- Multiple lacunar infarctions, which usually occur in both the gray matter and the deep hemispheric white matter.
- Cerebral infarction in key areas of the brain, such as the angular gyrus or thalamus.
- Subcortical arteriosclerotic encephalopathy.
- Thrombosis and embolism.
A study conducted by Dr. Constantino Ladecola, and published in the journal Neuron, points out the following:
Vascular dementia has as its origin an alteration in the blood vessels. However, this isn’t the only problem when it comes to sending oxygen and nutrients to the brain. There are also the changes suffered by neurons and glial cells, where the internal homeostasis changes, as does the communication between them.
Why does this neurodegenerative condition appear?
As we pointed out at the beginning, vascular dementia is related to certain risk factors. Thus, experts point out that, on average, this disease usually starts to show itself gradually around the age of 60. However, the symptoms become more evident from the age of 70 onwards. We should note that its onset is more common in men.
These are the triggers that are usually behind vascular dementia:
- Smoking.
- High blood pressure.
- High cholesterol.
- Diabetes.
- Obesity.
- Sedentary lifestyle.
- Having had heart problems.
- Having previously suffered a stroke.
- Vascular dementia also often has links with brain aging itself.
The symptoms of vascular dementia
The symptoms associated with vascular dementia are slow and progressive. Often, we interpret them as simple absent-mindedness or mood disturbances. However, there comes a time when the person’s functionality begins to be clearly affected and that’s when we should seek medical help and evaluation.
The most obvious symptoms are usually the following:
- Movement problems. The most obvious characteristics of a vascular problem are in the person’s movements, which are stiffer, slower, and clumsier.
- Problems in thinking. There are memory failures, and deficits in understanding, reflecting, paying attention, planning, and even following the flow of a conversation.
- Mood alterations. This characteristic is also very evident. The person suffers mood swings, is apathetic, unmotivated, angry, and sometimes may even show some aggressiveness. All of this can often be confused with depression when, in fact, there’s an irreversible underlying cause.
- Delusions and hallucinations.
It’s important to point out that the symptoms associated with vascular dementia may vary depending on the location of the infarcts or vascular alterations. Hence, we may at first see some clumsiness or even the inability to communicate. These realities can either appear suddenly or slowly.
What treatments are available for people with vascular dementia?
The damage caused by vascular dementia can’t be reversed, but it can be slowed down. Hence the importance of early detection, evaluation, and subsequent diagnostic imaging tests (CT scans, MRIs). Once the brain damage has been assessed, the factors that have triggered the condition, such as a heart problem, will be treated.
Doctors will adapt the treatment to each patient’s individual situation, and to which stage of the illness they find themselves in.
- Generally, a series of drugs are administered to treat the symptomatology and, in turn, to slow down the evolution of the disease.
- It’s also beneficial for the person to follow a neuro-rehabilitation program, where experts will train memory, comprehension, and attention.
- Multidisciplinary programs are always the most appropriate. Thus, the person can count on psychological assistance, physiotherapy, speech therapy, and even occupational therapy.
Family support is another element that we should take into account in all cases. We mustn’t forget that we’re facing realities that are as hard as they are exhausting, where emotions, resources, and demands come into play that we aren’t always prepared for.
Vascular dementia is, after Alzheimer’s, the most common neurodegenerative condition after the age of 70. The origin of this condition lies in blood flow problems, which make it difficult for blood to reach the brain. It’s somewhat slow and progressive but is something that greatly impacts a person’s quality of life, affecting their memory, movements, and communication.
We should note that, sadly, vascular dementia isn’t a reversible condition. Unfortunately, there’s no treatment to stop or effectively treat this harsh reality that hundreds of people and their families live. However, we can slow down its effects.
We should highlight one aspect at this point. Unlike Alzheimer’s, this type of dementia does have certain protective or precipitating factors, depending on the context, which we can all, to some extent, control.
This doesn’t mean that we can avoid it 100 percent, but it does mean that we can reduce its probability or delay its onset. We can relate vascular dementia to such well-known underlying factors as high blood pressure, cholesterol and triglycerides, diabetes, excess weight, an unhealthy lifestyle, etc.
Therefore, improving your vascular health is within your reach. We’re now going to have a look at the characteristics that define this disease, which accounts for about 20 percent of all dementia diagnoses.
Vascular dementia is the result of a repeated series of small strokes over time, which eventually lead to cognitive, mobility, and communication problems.

What’s vascular dementia?
Vascular dementia is a neurodegenerative disease that causes cognitive impairment. The origin lies in various vascular lesions and alterations, the most common being the following:
- A narrowing of the blood vessels in the brain, as a result of arteriosclerosis.
- Multiple lacunar infarctions, which usually occur in both the gray matter and the deep hemispheric white matter.
- Cerebral infarction in key areas of the brain, such as the angular gyrus or thalamus.
- Subcortical arteriosclerotic encephalopathy.
- Thrombosis and embolism.
A study conducted by Dr. Constantino Ladecola, and published in the journal Neuron, points out the following:
Vascular dementia has as its origin an alteration in the blood vessels. However, this isn’t the only problem when it comes to sending oxygen and nutrients to the brain. There are also the changes suffered by neurons and glial cells, where the internal homeostasis changes, as does the communication between them.

Why does this neurodegenerative condition appear?
As we pointed out at the beginning, vascular dementia is related to certain risk factors. Thus, experts point out that, on average, this disease usually starts to show itself gradually around the age of 60. However, the symptoms become more evident from the age of 70 onwards. We should note that its onset is more common in men.
These are the triggers that are usually behind vascular dementia:
- Smoking.
- High blood pressure.
- High cholesterol.
- Diabetes.
- Obesity.
- Sedentary lifestyle.
- Having had heart problems.
- Having previously suffered a stroke.
- Vascular dementia also often has links with brain aging itself.
The symptoms of vascular dementia
The symptoms associated with vascular dementia are slow and progressive. Often, we interpret them as simple absent-mindedness or mood disturbances. However, there comes a time when the person’s functionality begins to be clearly affected and that’s when we should seek medical help and evaluation.
The most obvious symptoms are usually the following:
- Movement problems. The most obvious characteristics of a vascular problem are in the person’s movements, which are stiffer, slower, and clumsier.
- Problems in thinking. There are memory failures, and deficits in understanding, reflecting, paying attention, planning, and even following the flow of a conversation.
- Mood alterations. This characteristic is also very evident. The person suffers mood swings, is apathetic, unmotivated, angry, and sometimes may even show some aggressiveness. All of this can often be confused with depression when, in fact, there’s an irreversible underlying cause.
- Delusions and hallucinations.
It’s important to point out that the symptoms associated with vascular dementia may vary depending on the location of the infarcts or vascular alterations. Hence, we may at first see some clumsiness or even the inability to communicate. These realities can either appear suddenly or slowly.
What treatments are available for people with vascular dementia?
The damage caused by vascular dementia can’t be reversed, but it can be slowed down. Hence the importance of early detection, evaluation, and subsequent diagnostic imaging tests (CT scans, MRIs). Once the brain damage has been assessed, the factors that have triggered the condition, such as a heart problem, will be treated.
Doctors will adapt the treatment to each patient’s individual situation, and to which stage of the illness they find themselves in.
- Generally, a series of drugs are administered to treat the symptomatology and, in turn, to slow down the evolution of the disease.
- It’s also beneficial for the person to follow a neuro-rehabilitation program, where experts will train memory, comprehension, and attention.
- Multidisciplinary programs are always the most appropriate. Thus, the person can count on psychological assistance, physiotherapy, speech therapy, and even occupational therapy.
Family support is another element that we should take into account in all cases. We mustn’t forget that we’re facing realities that are as hard as they are exhausting, where emotions, resources, and demands come into play that we aren’t always prepared for.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Iadecola, C. (2013, November 20). The Pathobiology of Vascular Dementia. Neuron. https://doi.org/10.1016/j.neuron.2013.10.008
- Caisberger, F., y Vališ, M. (2018). Demencia vascular. Interni Medicina pro Praxi , 20 (3), 159-162.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.







