Empty Sella Syndrome - Have You Heard About It?

The brain is still a mystery to humans. Therefore, scientific research does nothing but progress, and it’s constantly in search of new findings that’ll shed light on how it works. The literature is increasingly extensive and so is the knowledge about the brain. Today’s article is about sella turcica (Latin for Turkish seat), also known as empty sella syndrome (ESS).
Wait, what Turkish chair? You may be nodding your head right about now wondering what the heck this is all about. Others may be thinking: “Are there chairs inside the human head?” Furthermore, some people think “It sounds like something I’ve heard of”. Ok, for all of you, the oh-so-very peculiar name of sella turcica seems to be inspired by the shape of the frame of a saddle.
The causes of empty sella syndrome (ESS)
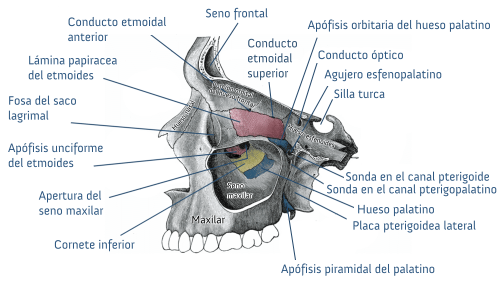
This is a brain structure occupied mostly by the pituitary gland and lives just below the base of the brain. When the pituitary flattens or shrinks, the area seems empty. You can’t see it on an MRI.
It’s full of cerebrospinal fluid that surrounds the spinal cord and brain. In cases of empty sella syndrome, the cerebrospinal fluid leaks into the saddle and presses on the pituitary by either flattening or shrinking it.
Primary empty sella syndrome
Primary empty sella syndrome is still under investigation. In this case, there’s no previous pathological process found at the moment. Neither its pathogenesis nor its clinical-surgical repercussions are clear, so the debates remain open. Even so, relevant data progressively shed more and more light.
Secondary empty sella syndrome
Secondary empty sella syndrome originates from a pathological process. It may or may not be of a tumor nature. In fact, it’s usually an adenoma (benign epithelial tumor) that later regresses in most cases. This involution occurs spontaneously or with treatment. As a result, the arachnoid cistern at the base of the skull goes into the empty space inside the sella turcica.
Who does it affect and what are its symptoms?
González-Tortosa (2009) highlights that patients are usually between the ages of 40 and 50. There’s a predominance in females with a high incidence of obesity. High blood pressure affects 23% of cases. 16.6% of these women are multiparous. In addition, it causes headache symptoms. Another characteristic symptom of idiopathic intracranial hypertension is a pulsating ringing in the ears.
According to the National Organization for Rare Disorders (NORD), “it’s unknown whether headaches develop because of empty sella syndrome or are simply a coincidental finding. Many individuals with empty sella syndrome have high blood pressure (hypertension), which can itself cause headaches if severe”.
Similarly, there may also be visual disturbances such as decreased visual acuity or blurred vision. Mental disturbances can also manifest. Above all, pictures of anxiety and alteration of behavior and dysthymia. In relation to endocrinological symptoms, there can be menstrual disturbances and sexual decrease in men.
Hypopituitarism
Hypopituitarism is a condition in the pituitary gland that causes the abnormal secretion of part or all of its hormones. The various hormones are prolactin, oxytocin, growth hormone, antidiuretic hormone, luteinizing hormone, etc.
Necochea’s team (1998) points out that supraventricular tachycardia (STV) may be one of the causes of hypopituitarism. Another common cause is “intrasellar or para-sellar tumors, such as pituitary adenomas, craniopharyngiomas, meningiomas, and lymphomas”. The authors also point to ischemic pituitary necrosis and pituitary ischemia due to vasculitis or diabetes mellitus.
Similarly, it can also be the result of an infection of the pituitary that could be caused by tuberculosis, brucellosis, syphilis, or mycosis. Also, of other diseases such as sarcoidosis, hemochromatosis, and histiocytosis.
Empty sella syndrome in children
González-Fernández’s team (2009) found symptomatic differences between adults and children with STV. One of these differences is that it isn’t present in obese children. There’s also no clear predominance of the sexes and the sella turcica isn’t enlarged. This suggests that different pathogenesis could occur in both.
As the authors point out, the hypothalamic-pituitary function is another difference. Generally, the hypogonadotropic hypogonadism (HH) hormonal function doesn’t alter in adult patients, although it isn’t absolutely exempt from being there. The authors place special emphasis on the study of HH hormonal function as it occurs more frequently in children than in adults.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








