Pachygyria: The "Smooth" Brain
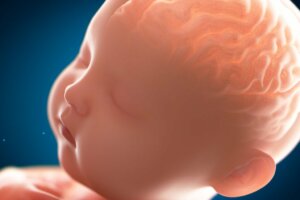
Pachygyria is a congenital malformation of the cerebral cortex. It results from poor neuronal migration, causing abnormally thick convolutions.
Generally speaking, children with pachygyria tend to have a variable degree of intellectual disability. Other main symptoms would be developmental delays and seizure disorders.
But what’s the cause of pachygyria? How is it diagnosed and what are its symptoms? Does it have treatment? Keep reading to find out!
What’s the cerebral cortex and what does it look like?
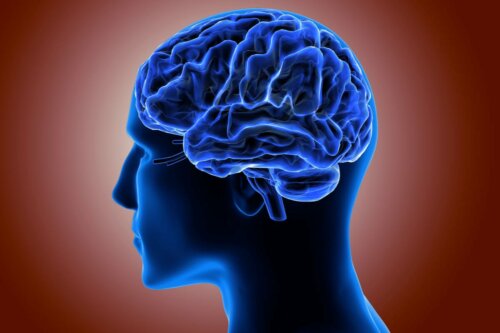
The cerebral cortex covers the surface of the two cerebral hemispheres. The cortex has a very folded structure, which makes it possible for it to have a large surface area in a small space compared to the surface of a smooth brain of the same size.
Moreover, on the surface of the cortex, you can distinguish two things. Firstly, fissures, which are furrows of variable size. Secondly, convolutions, which are bulges located between the clefts.
The cortex mainly consists of glial cells and neuronal bodies. It’s organized into six layers in which neurons are precisely arranged.
Pachygyria: what is it exactly?
Pachygyria is a malformation that belongs to the family of lissencephaly. To clarify, the latter refers to disorders characterized by a smoothing of the surface of the cortex. It’s found between agyria (the total absence of convolutions), and polymicrogyria (a malformation of the cortex that presents excessive convolutions).
Furthermore, pachygyria is a serious congenital malformation with a fairly high mortality rate. In it, there’s an alteration of the organization of the neurons of the cerebral cortex and its structure. It causes the cerebral cortex to be thinner than normal because some of the six layers that make up the cortex are absent or their cells aren’t organized properly.
In addition, the main characteristic is that the cortex has little pronounced fissures and thicker and wider convolutions than normal. This, as a result, makes the cortex look smoother (less “folded”).
The symptoms of pachygyria
The most common symptoms that children with pachygyria present are the following. Intellectual disability, seizures, and severe developmental impairment. However, there are other symptoms worth mentioning:
- Epileptic seizures (present in 90% of children). They usually appear between the fourth and seventh month of age. These are quite resistant to treatment which, evidently, puts the child’s life at risk.
- Developmental delay and disturbances, both in motor development and in language development. These children usually present hypotonia in their extremities, which makes it difficult for them to walk and stay upright, as well as poor language. Additionally, they usually have microcephaly.
- Severe to profound intellectual disability that limits the child’s cognitive functions and autonomy.
- Behavioral disorders and other mental disorders.
Diagnosis
The absence of characteristic facial or physical features can hinder the diagnostic process. Therefore, the diagnosis is based on the clinical examination of the symptoms and on neuroimaging techniques that allow medical professionals to evaluate the cerebral cortex in a more detailed way.
CAT scans (computerized axial tomography) provide images of the brain with high spatial resolution. However, the malformations of the cortex are easier to visualize in vivo. For that reason, magnetic resonance imaging is more useful as it offers greater contrast and better differentiation of gray and white matter.
In the images, it’s possible to see thickened cerebral convolutions with few shallow clefts, as well as the incomplete development of the Sylvian fissure.
The causes of pachygyria
The cause of this condition is a disruption in the fetal neuronal migration process. Environmental influences or genetic alterations may cause this failure. Let’s address this.
Neuronal migration occurs between the seventh and 20th week of gestation. The goal of this migration is to form the six layers that make up the cortex. However, in pachygyria, only four of the six layers are present, making the cortex thinner than normal.
Moreover, in a brain with pachygyria, the first layer (molecular or plexiform) is present and is the same as in a normal brain. However, the second, third, and fourth layers have fewer cells than a healthy brain, as well as a thinner structure.
As we mentioned above, environmental influences can cause this alteration in neuronal migration. For example, exposure to certain substances or elements (radiation, alcohol, and mercury, among others).
The genetic alterations responsible for pachygyria are too complex for us to address in this article. However, we must point out that the most common genetic alterations that cause pachygyria are usually related to the X chromosome and the 17th chromosome. Likewise, the absence of the LIS1 gene seems to be the cause of lissencephaly.
Lack of treatment
As in almost all rare diseases, only symptomatic treatment exists. In this case, the administration of antiepileptic drugs to treat seizures is essential.
As you can see, this is a serious malformation that causes the death of most children born with it. However, when this malformation doesn’t affect the cortex, it’s compatible with life and the child’s involvement will depend on the region affected by it.
In case the child survives, it’s imperative to work with different professionals, from physiotherapists who help to work on motor disorders such as hypotonia, to special education teachers who carry out a curricular adaptation for the child’s education.
Of course, those aren’t the only professionals to work with, as doctors, nurses, occupational therapists, and psychologists are essential. They can improve the quality of the child’s life and help them become as autonomous as they possibly can.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
Vélez-Domínguez, L. C. (1998). Transtornos de migration neuronal. Gac Med Mex, 134(2), 207-15.
HERNÁNDEZ CH, M. A. R. T. A., Bolte, L., Mesa, T., Escobar, R., Mellado, C., & Huete, I. (2007). Lisencefalia y epilepsia en pediatría. Revista chilena de pediatría, 78(6), 615-620.
Pérez-Jiménez, A., Colamaria, V., Franco, A., Grimau-Merino, R., Darra, F., & Fontana, E. (1998). Epilepsia y alteraciones del desarrollo cortical enVallejo Desviat, P., & Hernández Sánchez, G.
MALFORMACIONES CONGÉNITAS POR ALTERACIÓN EN EL DESARROLLO DE LA CORTEZA CEREBRAL. REVISIÓN DE CASOS EN LOS ÚLTIMOS 5 AÑOS. niños con infección congénita por citomegalovirus. Rev Neurol, 26(149), 42-49.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








